When your heart muscle stops working the way it should, it doesn’t just feel like fatigue-it can be life-threatening. Cardiomyopathy isn’t one disease. It’s a group of conditions that change the structure and function of your heart muscle, making it harder to pump blood. The three main types-dilated, hypertrophic, and restrictive-each behave differently, affect different people, and need totally different treatments. Knowing which one you’re dealing with isn’t just medical jargon; it’s the difference between managing symptoms and preventing sudden cardiac arrest.
Dilated Cardiomyopathy: The Enlarged, Weak Pump
Dilated cardiomyopathy (DCM) is the most common form, making up about half of all cases. Imagine your heart’s main pumping chamber, the left ventricle, stretching out like an overinflated balloon. The walls get thin, the chamber grows too large, and the muscle loses its grip. Instead of squeezing hard, it just flops. This leads to poor blood flow, fluid buildup in the lungs and legs, and eventually heart failure.
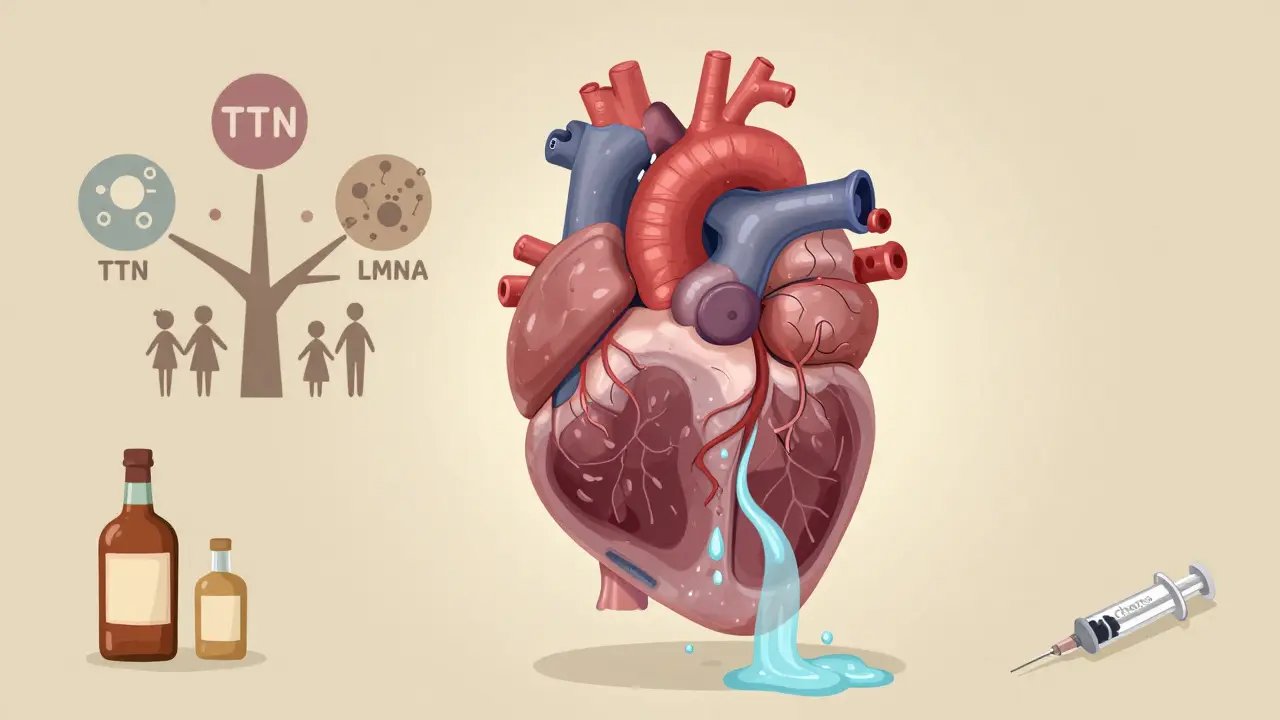
It’s not always clear why this happens. In about one-third of cases, it runs in families-mutations in genes like TTN or LMNA are often to blame. But in many others, it’s triggered by outside factors: long-term heavy drinking (more than 80 grams of alcohol a day for five years or more), viral infections like coxsackievirus, or chemotherapy drugs such as doxorubicin. Even autoimmune diseases like sarcoidosis can silently damage the heart muscle over time.
Doctors diagnose DCM with an echocardiogram. If the left ventricle is bigger than 55 mm in men or 50 mm in women, and the ejection fraction (how much blood it pumps out) drops below 40%, that’s a clear signal. Cardiac MRI adds more detail, showing scar tissue or inflammation that an echo might miss. Treatment isn’t about fixing the size-it’s about helping the heart work better. Guideline-directed medical therapy (GDMT) includes drugs like sacubitril/valsartan, beta-blockers, and SGLT2 inhibitors. These don’t reverse the damage, but they cut death risk by 30% over three years. In severe cases, an implantable defibrillator or even a heart transplant becomes necessary.
Hypertrophic Cardiomyopathy: The Thickened, Stiff Heart
If DCM is about stretching, hypertrophic cardiomyopathy (HCM) is about thickening. The heart muscle, especially the wall between the two lower chambers (the septum), grows abnormally thick-often over 15 mm. This isn’t from high blood pressure or exercise. It’s genetic. About 60% of cases come from mutations in sarcomere genes like MYH7 or MYBPC3, passed down in an autosomal dominant pattern. That means if one parent has it, each child has a 50% chance of inheriting it.
What makes HCM dangerous isn’t just the thickness. It’s how it blocks blood flow. In 70% of cases, the thickened septum gets in the way of blood leaving the heart, creating a pressure gradient over 30 mmHg. This is called obstructive HCM. The heart works harder, oxygen demand spikes, and arrhythmias can strike. It’s the top cause of sudden death in young athletes under 35 in the U.S., responsible for nearly a third of those cases.
Diagnosis starts with an echo. If the septum is thick and there’s no other explanation, HCM is suspected. Genetic testing confirms it in about 60% of cases, using a 17-gene panel that costs $1,200-$2,500 in the U.S. But not everyone with the gene gets sick-penetrance is incomplete. That’s why family screening matters. Treatment focuses on reducing symptoms and preventing sudden death. Beta-blockers help most patients, easing shortness of breath and chest pain. For those with severe obstruction, disopyramide or septal reduction (surgery or alcohol ablation) can open the flow. In 2022, the FDA approved mavacamten (Camzyos), a first-of-its-kind drug that directly targets the overactive heart muscle, cutting outflow gradients by 80% in trials. Still, 42% of HCM patients report ongoing symptoms despite treatment.

Restrictive Cardiomyopathy: The Stiff, Non-Compliant Chamber
Restrictive cardiomyopathy (RCM) is the rarest-only 5% of cases-but often the hardest to catch. Unlike the others, the heart muscle doesn’t get weak or thick. It gets stiff. Think of it like a rubber band that lost its stretch. The chambers stay small, the pumping strength (ejection fraction) stays normal, but the heart can’t fill with blood properly. Blood backs up into the lungs and liver, causing swelling, fatigue, and fluid retention.
RCM isn’t usually inherited. It’s caused by things that infiltrate the heart tissue: amyloidosis (60% of cases), where abnormal proteins build up like sludge; sarcoidosis (15%), where immune cells form clumps; hemochromatosis (10%), where iron overloads the organs; or rare storage diseases like Fabry disease. The key clue? Normal systolic function with severe diastolic dysfunction. On echo, you’ll see a fast, sharp filling pattern-E/A ratio over 2 with deceleration time under 150 milliseconds.
Diagnosing RCM is tricky because it mimics constrictive pericarditis, where the sac around the heart hardens. The difference? RCM is inside the muscle; constriction is outside. Cardiac MRI is essential here. Late gadolinium enhancement in a non-coronary pattern, plus extracellular volume over 35%, points to fibrosis or infiltration. An endomyocardial biopsy may be needed to confirm amyloidosis or sarcoidosis.
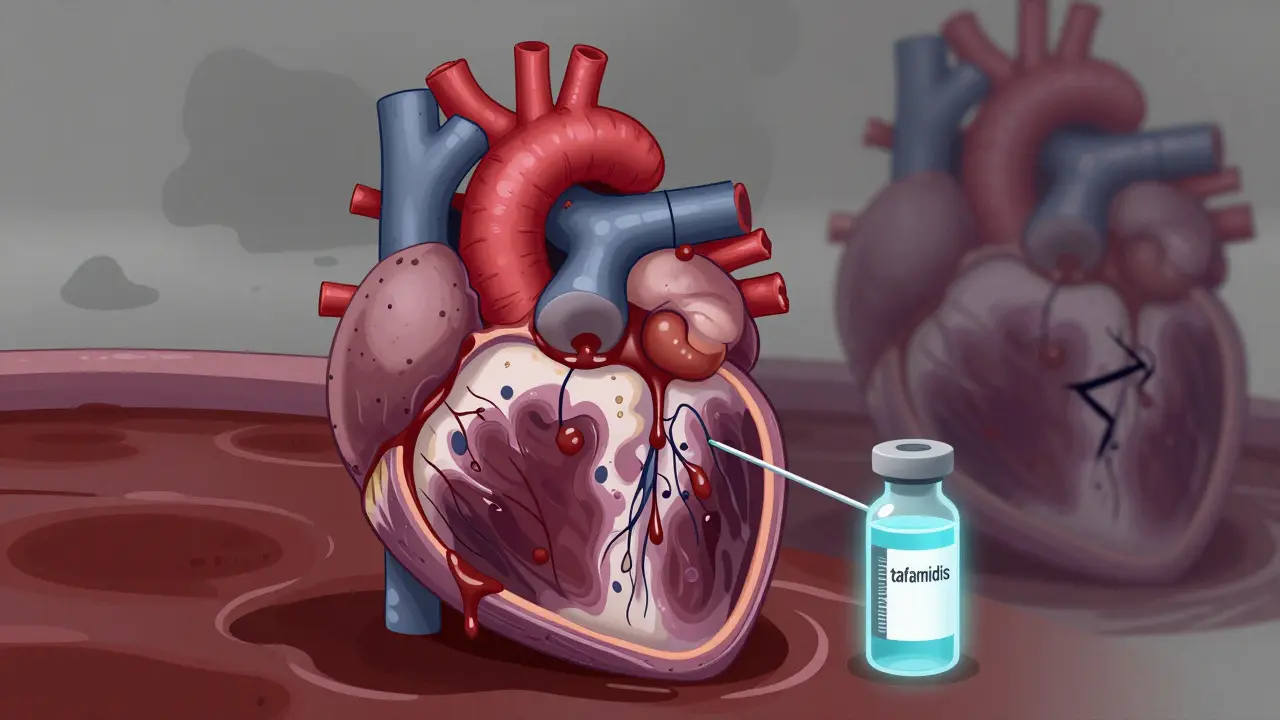
Treatment targets the root cause. For light-chain amyloidosis, drugs like daratumumab can stop protein buildup. For hemochromatosis, regular phlebotomy (blood removal) helps. Tafamidis, used for transthyretin amyloidosis, improves walking distance by 25 meters in trials-but costs $225,000 a year in the U.S. Prognosis is grim without treatment: 30-50% five-year survival, depending on the cause. Even with treatment, RCM lags behind the others in survival gains.
Why Classification Matters
Doctors used to group all heart muscle diseases together. Now, we know that mislabeling DCM as ischemic (from blocked arteries) leads to wrong treatments. The 2020 American Heart Association guidelines made it clear: if coronary disease is the cause, it’s not cardiomyopathy-it’s coronary artery disease with heart failure. This shift means more accurate diagnosis and better outcomes.
For patients, this matters. A person with HCM needs strict activity limits and genetic counseling for their kids. Someone with RCM from amyloidosis needs a specialist who knows about tafamidis or daratumumab. And a person with DCM needs to know whether their condition is genetic, because their siblings might need screening.
Research is moving fast. CRISPR-based gene editing for HCM (VERVE-201 trial) is entering Phase I in 2024. Polygenic risk scores, which combine dozens of small genetic signals, could predict HCM before symptoms appear by 2026. But access is uneven. Only 35% of community hospitals correctly classify these types, and rural areas often lack specialists. In Australia, where I live, access to advanced diagnostics like cardiac MRI and genetic panels is better in cities but still limited in regional areas.
What You Can Do
If you’ve been told you have cardiomyopathy, ask: Which type? Ask for an echo and MRI. Ask if genetic testing is recommended. Ask about family screening. Don’t assume all heart failure is the same.
If you have a family history of sudden cardiac death before age 40, or unexplained heart failure, get checked. Early detection saves lives-especially in HCM, where 90% of sudden deaths happen in undiagnosed people.
And if you’re struggling with symptoms-shortness of breath, swelling, dizziness-don’t wait. The right diagnosis opens the door to the right treatment. Whether it’s a daily pill, a new drug, or a device, knowing the type of cardiomyopathy you have isn’t just academic. It’s your lifeline.
Can cardiomyopathy be cured?
There’s no cure for most types of cardiomyopathy, but treatments can manage symptoms and slow progression. Dilated cardiomyopathy responds well to medications like sacubitril/valsartan and SGLT2 inhibitors, reducing death risk by 30%. Hypertrophic cardiomyopathy can be controlled with beta-blockers or surgery, and some patients live normally. Restrictive cardiomyopathy’s outcome depends on the cause-treating amyloidosis or hemochromatosis can improve survival. In advanced cases, a heart transplant may be the only option.
Is cardiomyopathy hereditary?
Yes, in many cases. About 25-35% of dilated cardiomyopathy, 60% of hypertrophic cardiomyopathy, and some cases of restrictive cardiomyopathy (like Fabry disease) have genetic causes. If a close family member has cardiomyopathy, especially if they died suddenly or were diagnosed young, other relatives should be screened. Genetic testing can identify mutations, and regular echocardiograms can catch early signs before symptoms appear.
Can exercise make cardiomyopathy worse?
It depends on the type. For hypertrophic cardiomyopathy, intense or competitive sports can trigger sudden cardiac arrest-so strenuous activity is usually restricted. For dilated cardiomyopathy, moderate aerobic exercise (like walking or cycling) is encouraged as it improves heart function and reduces symptoms. Restrictive cardiomyopathy patients should avoid heavy lifting and extreme exertion, as it increases pressure on the stiff heart. Always consult a cardiologist before starting or changing an exercise routine.
How is restrictive cardiomyopathy different from constrictive pericarditis?
Both conditions cause similar symptoms-swelling, fatigue, shortness of breath-but they’re treated completely differently. Restrictive cardiomyopathy is a disease of the heart muscle itself, made stiff by infiltration (like amyloid proteins). Constrictive pericarditis is caused by a hardened sac around the heart. The key difference? In constriction, the heart muscle is normal, and removing the stiff outer layer (pericardiectomy) can cure it. In restrictive, the muscle is damaged, and treatment targets the underlying cause. Cardiac MRI and tissue biopsy are needed to tell them apart.
What’s the latest treatment for hypertrophic cardiomyopathy?
The biggest recent advance is mavacamten (Camzyos), approved by the FDA in 2022. It’s the first drug designed specifically for obstructive HCM. It works by reducing the force of heart muscle contractions, lowering the pressure gradient by up to 80% in clinical trials. It’s taken orally and has shown major improvements in exercise capacity and symptoms. Before this, treatment was limited to beta-blockers, calcium channel blockers, or invasive procedures. Mavacamten costs about $145,000 per year in the U.S., but it’s changing the standard of care for those with persistent symptoms.


I don't trust these so-called experts. They say DCM is genetic but what about the 5G towers and the vaccines? They're hiding the real cause. Your heart doesn't just fail for no reason. Something's being covered up. I've seen too many cases where people got sick right after their checkup. Don't believe the system.