If you live with Meniere’s disease, you know the sudden dizziness, the ringing in your ears, and the feeling that your head is full of cotton. These episodes don’t just come out of nowhere-they’re often tied to what’s happening inside your body, especially in your inner ear. The good news? What you eat and drink can make a real difference. For decades, doctors have pointed to two simple, powerful tools: cutting back on sodium and drinking the right amount of water. This isn’t guesswork. It’s backed by research, patient outcomes, and clinical guidelines from leading medical groups.
Why Sodium Matters for Your Inner Ear
Your inner ear isn’t just a hearing organ-it’s a fluid-filled chamber called the endolymphatic sac a structure in the inner ear that regulates fluid pressure and ion balance. When too much fluid builds up-what doctors call endolymphatic hydrops an abnormal accumulation of fluid in the inner ear that causes pressure and disrupts balance and hearing-it triggers the classic symptoms of Meniere’s: vertigo, muffled hearing, tinnitus, and pressure.
Sodium is the main reason this fluid builds up. When you eat salt, your body holds onto water to keep your blood sodium levels stable. That extra fluid doesn’t just stay in your bloodstream-it leaks into your inner ear. Think of it like a sponge soaking up water. The more sodium you take in, the more your inner ear swells. That swelling is what causes the attacks.
Studies show that people with Meniere’s who cut sodium see measurable improvements. A 2024 study in Acta Otolaryngologica followed 50 patients who stuck to a 1,500 mg sodium limit and drank 35 ml of water per kilogram of body weight daily. After six months, their hearing improved by an average of 12.3 decibels at key frequencies. Their vertigo attacks dropped by nearly half. Tinnitus got quieter. The pressure in their ears lessened. This wasn’t a small change-it was a life-altering shift for most participants.
How Much Sodium Is Too Much?
Most health agencies agree: for Meniere’s, less is better. But how much less?
- 1,500 mg per day is the target recommended by the 2024 Acta Otolaryngologica a peer-reviewed medical journal that published Level 1 evidence on sodium restriction for Meniere's disease study and supported by the American Heart Association a leading U.S. organization that recommends 1,500 mg daily sodium for optimal cardiovascular and inner ear health.
- 2,000 mg per day is the upper limit suggested by the Mayo Clinic a trusted U.S. medical institution that recommends sodium restriction as first-line therapy for Meniere's disease and the National Institutes of Health a U.S. government agency that funds and publishes research on Meniere's disease and dietary interventions.
- 2,300 mg per day is the general U.S. dietary limit for healthy adults-but for Meniere’s, this is too high.
That’s about ¾ to 1 teaspoon of salt. Sounds simple, right? But here’s the catch: most of the sodium you eat isn’t from the salt shaker. Over 77% comes from packaged and restaurant food. A single slice of deli meat can have 600 mg. A bowl of canned soup? 900 mg. A burger and fries? Easily over 1,500 mg before you even add salt.
Fluid Balance: Drink More Water (Yes, Really)
You’ve probably heard, “Avoid fluids if you have Meniere’s.” That’s outdated advice. In fact, the opposite is true.
When you restrict sodium but don’t drink enough water, your body goes into survival mode. It holds onto every drop of fluid it can-right in your inner ear. That’s why some people see no improvement even on a low-salt diet: they’re dehydrated.
The 2024 study gave patients a clear target: 35 ml of water per kilogram of body weight per day. For someone weighing 70 kg (154 lbs), that’s about 2.5 liters-roughly 10 glasses. Not all at once. Spread it out. Sip throughout the day.
Why does this work? Stable hydration helps your kidneys flush out excess sodium more efficiently. It also keeps your inner ear fluid from becoming too concentrated. Think of it like balancing a scale. Sodium pulls water in. Water helps flush it out. You need both.
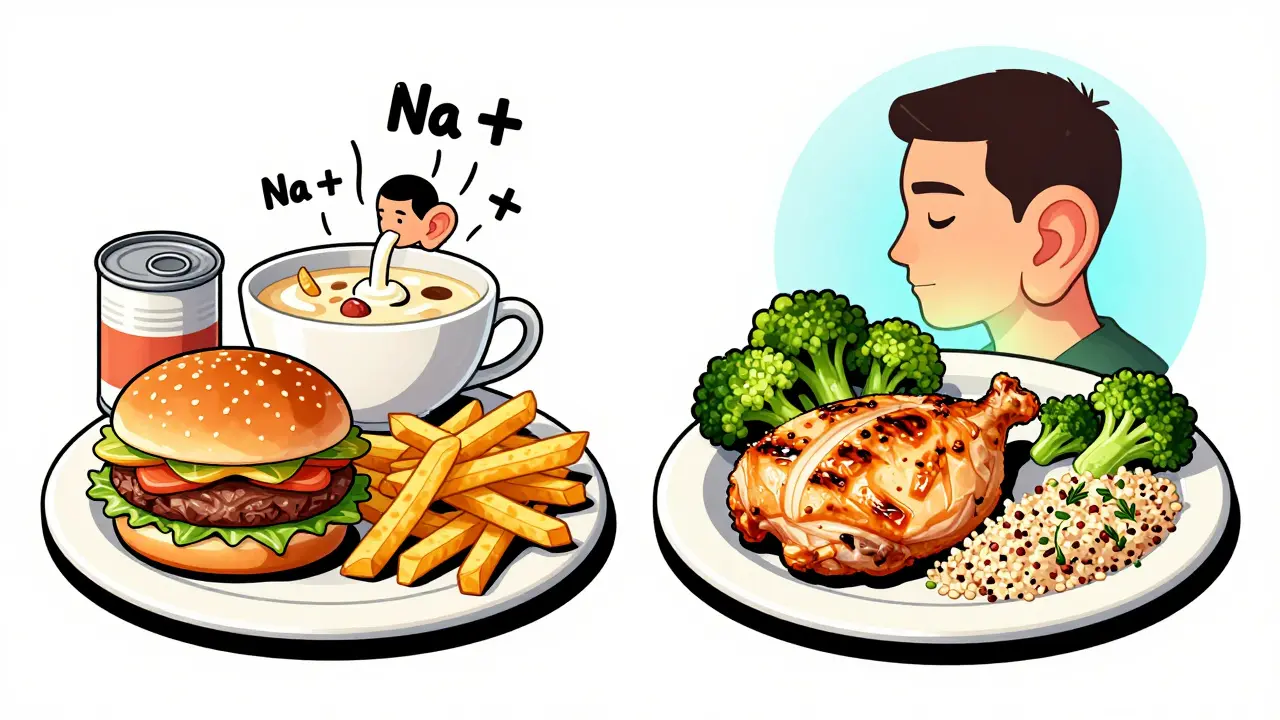
What to Eat (and What to Avoid)
Switching to a low-sodium diet doesn’t mean eating bland food. It means eating smarter.
Do This:
- Choose fresh fruits, vegetables, lean meats, and plain grains. These have almost no added sodium.
- Use herbs, lemon juice, garlic, vinegar, and salt-free spice blends instead of salt.
- Check labels. Look for “no salt added,” “low sodium,” or “sodium-free.” Anything under 140 mg per serving is considered low.
- Buy frozen vegetables without sauce. Canned beans rinsed under water lose up to 40% of their sodium.
- When dining out, ask for meals prepared without salt. Most restaurants will accommodate you.
Avoid These:
- Processed meats: bacon, ham, salami, hot dogs
- Sauces: soy sauce, ketchup, mustard, Worcestershire sauce, barbecue sauce
- Snacks: chips, pretzels, salted nuts, crackers
- Fast food: burgers, fries, pizza, tacos
- Canned soups and broths
- Pre-packaged meals: frozen dinners, instant noodles, rice mixes
One patient I spoke with in Melbourne-let’s call her Lisa-used to eat canned soup for lunch every day. She cut it out, started making vegetable stew with fresh tomatoes and herbs, and within three weeks, her vertigo attacks dropped from three times a week to once a month. She didn’t need more medication. Just better food.
Other Triggers: Caffeine, Alcohol, and Sugar
Sodium isn’t the only player. Caffeine and alcohol can make symptoms worse.
Caffeine-found in coffee, tea, energy drinks, and chocolate-narrows blood vessels. That includes the tiny vessels in your inner ear. Reduced blood flow means less oxygen and nutrients for the delicate hair cells that help you hear and balance. Many patients report fewer attacks when they cut caffeine to one cup a day or less.
Alcohol affects your inner ear fluid directly. It changes the composition of the fluid and can trigger dizziness even hours after drinking. Most experts recommend avoiding it entirely, especially during flare-ups.
Sugar? It’s sneaky. High sugar intake spikes insulin, which can interfere with sodium excretion. It also causes inflammation. A 2023 review in Frontiers in Nutrition noted that patients who reduced sugar saw a secondary improvement in tinnitus, even if they weren’t focused on it.
Why Diet Beats Pills (At Least at First)
Doctors often prescribe diuretics like hydrochlorothiazide or acetazolamide. These drugs help flush out fluid. But they come with side effects: low potassium, dizziness, kidney stones, fatigue.
Compare that to dietary changes. No side effects. No prescription refill. Just you, your kitchen, and a little patience.
A 2020 study found that 68% of Meniere’s patients saw major improvement on a low-salt diet-without drugs. That’s better than the 50-70% success rate for diuretics. And it’s safer. For many, diet alone is enough to control symptoms for years.
Of course, it’s not magic. It takes effort. You have to read labels. You have to cook more. You have to say no to pizza night. But for most people, the payoff is worth it: fewer dizzy spells, clearer hearing, quieter ears.

What If Diet Doesn’t Work?
Not everyone responds. About 22% of patients struggle to stick with the diet long-term. Social events, work lunches, family habits-it’s hard to change everything overnight.
If your symptoms don’t improve after 3-6 months of strict sodium and fluid control, talk to your ENT specialist. Options include:
- Intratympanic steroid injections (dexamethasone): Reduce inflammation directly in the ear. About 60-75% effective.
- Gentamicin injections: Destroy part of the balance nerve. 80-90% effective for vertigo-but carries a risk of hearing loss.
- Surgery: Reserved for severe, disabling cases that don’t respond to anything else.
But here’s the thing: even if you need one of these later, starting with diet gives you the best foundation. It reduces the severity of your symptoms, so you need less aggressive treatment down the road.
Getting Started: A Simple 7-Day Plan
Don’t try to overhaul your whole life in one week. Start here:
- Day 1-2: Toss the salt shaker. Replace it with black pepper, garlic powder, or lemon zest.
- Day 3-4: Replace one high-sodium food with a low-sodium alternative. Swap canned soup for homemade vegetable broth.
- Day 5: Buy a food scale or use a nutrition app to track sodium for one day. You’ll be shocked at how fast it adds up.
- Day 6: Drink 35 ml of water per kg of body weight. Set phone reminders if you need to.
- Day 7: Plan one low-sodium meal. Try grilled chicken, steamed broccoli, and quinoa with herbs.
After seven days, you’ll have a new routine. You won’t miss the salt. You’ll start noticing how much better you feel.
Final Thought: This Is Your Tool, Not Your Prison
Meniere’s doesn’t have a cure. But this? This is control. You can’t always stop an attack. But you can reduce how often they happen-and how hard they hit.
Low sodium. Clean water. Real food. No magic pills. No risky procedures. Just you, making smarter choices every day. It’s not easy. But it’s one of the few things in Meniere’s care that actually works-for most people, most of the time.
Start today. Not tomorrow. Today. Your ears will thank you.
Can I still eat out if I have Meniere’s disease?
Yes, but you need to be strategic. Ask for meals prepared without salt or added sauces. Choose grilled proteins, steamed vegetables, and plain rice or potatoes. Avoid fried foods, soups, and anything with a sauce or glaze. Most restaurants will accommodate you if you ask politely. Consider eating at places that focus on fresh ingredients, like salad bars or sushi spots (without soy sauce).
Is sea salt or kosher salt better than table salt for Meniere’s?
No. All types of salt-sea salt, kosher salt, Himalayan salt-are made of sodium chloride. They contain the same amount of sodium per gram. The texture might be different, but your body processes it the same way. If you’re limiting sodium, you’re limiting all salt, regardless of the label.
How long does it take to see results from a low-sodium diet?
Some people notice less dizziness or quieter tinnitus within 2-3 weeks. But for full improvement in hearing and attack frequency, most studies show you need at least 3-6 months of consistent sodium restriction. Don’t give up if you don’t see changes right away. Your inner ear takes time to rebalance.
Can I drink alcohol occasionally if I have Meniere’s?
It’s best to avoid alcohol entirely. Even small amounts can trigger or worsen vertigo, tinnitus, and ear pressure. Alcohol changes the fluid composition in your inner ear and can cause dehydration. If you do choose to drink, limit it to one small glass on rare occasions-and never on days when you feel unwell.
Do I need to take supplements if I cut out salt?
Not usually. A balanced, whole-food diet with plenty of fruits, vegetables, lean proteins, and healthy fats provides all the nutrients you need. Avoid potassium supplements unless your doctor recommends them-too much potassium can be dangerous. If you’re worried about nutrient gaps, talk to a dietitian who specializes in Meniere’s or vestibular disorders.


Bro, I was skeptical too-until I cut salt and started sipping water like it was my job. Three weeks in, my vertigo went from daily to once a month. No meds. No shots. Just me, my kitchen, and a damn water bottle. If you’re still eating canned soup or deli meat, you’re fighting your own body. Stop. Just stop. 🤞