Living with chronic pain can feel like you are trapped in a loop of medications that stop working and surgeries that leave you worse off. If you have tried everything else without relief, spinal cord stimulation might be the missing piece of your puzzle. This medical treatment uses gentle electrical pulses to interrupt pain signals before they reach your brain. But it is not for everyone. Understanding who qualifies as a candidate and what the process involves can save you time, money, and unnecessary suffering.
What Is Spinal Cord Stimulation?
Spinal cord stimulation (SCS) is a neuromodulation technique that delivers pulsed electrical energy via implanted electrodes to manage chronic, intractable pain. Think of it as a pacemaker for your nerves. Instead of stopping the heart from beating irregularly, an SCS device stops your nervous system from sending "pain" messages to your brain. The technology has evolved significantly since its development in 1967 by Dr. C. Norman Shealy. Modern systems are far more sophisticated, offering different types of stimulation that can target specific pain patterns without the buzzing sensation older devices caused.
The core components of an SCS system include leads (thin wires with electrodes), a connector, and an implantable pulse generator (IPG), which acts as the battery and computer. These devices sit in the epidural space-the area just outside the protective covering of the spinal cord. By placing electrodes here, doctors can precisely target the dorsal columns of the spinal cord where sensory information travels. This approach sits in the middle of the pain management spectrum. It is more invasive than injections or pills but less risky than major spinal fusion surgeries.
How Does Spinal Cord Stimulation Work?
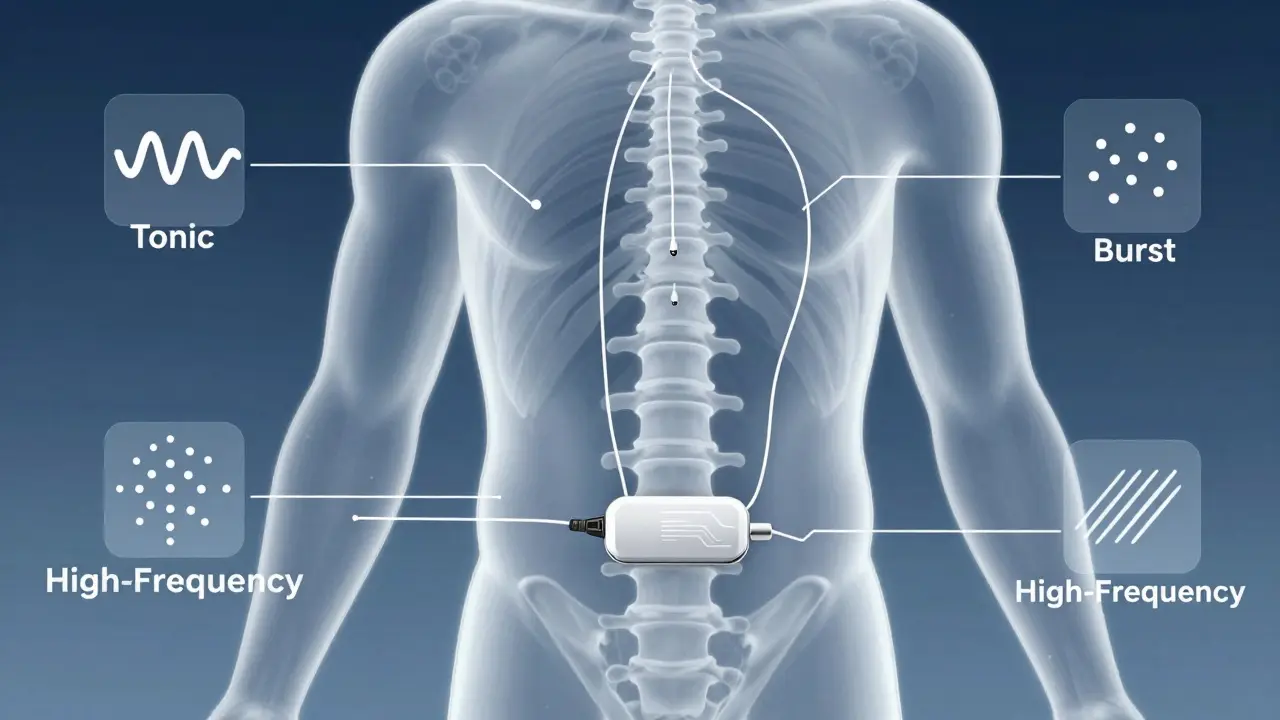
The magic happens through electrical modulation. When the device fires, it sends low-level electrical currents that override pain signals. You might feel a mild tingling sensation, known as paresthesia, in the areas where you used to feel pain. For many patients, this tingling completely masks the discomfort. However, newer technologies have changed the game. High-frequency stimulation operates at speeds between 1,000 and 10,000 Hz, providing pain relief without any tingling sensation. Burst stimulation mimics natural neuronal firing patterns, sending quick trains of pulses that feel more natural to the body.
Two main methods deliver this current: constant voltage and constant current. Constant voltage creates spike-shaped pulses that can become sharper if tissue resistance increases. Constant current produces smooth, rectangular pulses that stay consistent regardless of impedance changes. A 2019 study at Mayo Clinic found that 68% of patients preferred constant current because it felt more comfortable and provided better pain control. Manufacturers like Boston Scientific, Medtronic, and Abbott offer various platforms, such as the Precision™ System, Intellis™ platform, and Proclaim™ systems, each with unique waveform capabilities.
| Type | Frequency Range | Sensation | Best For |
|---|---|---|---|
| Tonic (Traditional) | 30-120 Hz | Mild tingling (paresthesia) | Localized neuropathic pain |
| Burst | 500 Hz bursts at 40 Hz | No tingling, rhythmic pulse | Pain unresponsive to tonic stimulation |
| High-Frequency | 1,000-10,000 Hz | No sensation (paresthesia-free) | Axial back pain, CRPS |
Who Is a Good Candidate for SCS?
Not everyone with chronic pain should get an SCS implant. In fact, failure rates can exceed 40% if screening protocols are ignored. The ideal candidate has exhausted conservative treatments over a period of 12 to 24 months. This includes physical therapy, medication adjustments, and minimally invasive procedures. Your pain must be clearly defined, meaning you can point to exactly where it hurts-often described as burning, shooting, or electric shock-like sensations typical of neuropathic pain.
Psychological health plays a huge role in success. Dr. Robert Levy, past president of the International Neuromodulation Society, notes that untreated major depression lowers success rates by 35%. Pain is complex, involving both physical and emotional pathways. Patients need realistic expectations. SCS rarely eliminates 100% of pain; the goal is usually a 50% reduction or greater. This level of relief allows people to walk further, sleep better, and reduce opioid use. According to a 2021 JAMA Network Open study, SCS recipients had 57% lower opioid utilization at one year compared to those on optimized medical management alone.
Common conditions that respond well to SCS include:
- Failed Back Surgery Syndrome (FBSS): Pain persisting after spinal surgery, accounting for about 52% of cases.
- Complex Regional Pain Syndrome (CRPS): Types I and II, formerly known as RSD and causalgia, representing roughly 24% of implants.
- Intractable low back and leg pain due to degenerative disc disease or stenosis.
- Peripheral nerve injuries causing localized neuropathic pain.
If you cannot operate the device, fail trial stimulation, or are pregnant, you are likely not a candidate. Safety ratings from the Washington State Health Care Authority label SCS efficacy as "High" but safety as "Medium" due to revision risks, making careful patient selection critical.
The Implantation Process: Trial to Permanent
You do not jump straight into permanent surgery. The process starts with a trial phase lasting 5 to 7 days. Under sedation and fluoroscopic guidance, a doctor places temporary percutaneous leads in your epidural space. These connect to an external pulse generator worn on your skin. During this week, you go about your daily life while adjusting settings to find the sweet spot for pain relief. If you achieve at least 50% pain reduction, the trial is considered successful.
If the trial works, you proceed to permanent implantation. This is a 60- to 90-minute surgical procedure. The surgeon places permanent leads in the epidural space and connects them to an IPG, which is placed under the skin in your abdomen or buttock. Recovery varies, but most people return to light activities within a few days. Learning to program the device takes 2 to 4 weeks. About 89% of patients need at least one follow-up programming session with their physician to fine-tune the settings.
Risks, Costs, and Long-Term Outlook
Like any surgery, SCS carries risks. Lead migration occurs in about 15.3% of cases within six months, which can cause intermittent stimulation or loss of coverage. Infection rates range from 3.8% to 7.2%, sometimes requiring removal of the device. Battery replacement is another consideration. Most IPGs last 5 to 9 years, requiring a minor outpatient surgery to swap the battery. Newer models, like the WaveWriter Alpha™ Prime, boast up to 24-month battery life, reducing these interventions.
Cost is a significant factor. The total price for the system and implantation ranges from $25,000 to $45,000 in the U.S. Medicare covers approved indications like FBSS and CRPS, but patients often face out-of-pocket costs of $15,000 to $25,000 depending on insurance plans. Despite the expense, many report saving money long-term by cutting down on medications. One group of patients noted reducing monthly medication costs by $800 after implantation.
Long-term efficacy data shows mixed results. While 76% of patients maintain significant pain relief at six months, only 58% keep that level of relief at three years. A 2022 meta-analysis suggested that placebo effects may diminish over time, leaving 52% of patients with meaningful relief at five years. This highlights the importance of ongoing management and realistic expectations.
Alternatives to Spinal Cord Stimulation
If SCS isn't right for you, other options exist. Transcutaneous Electrical Nerve Stimulation (TENS) units cost only $50 to $200 and are non-invasive, but they provide much less effective relief for severe chronic conditions. Peripheral nerve field stimulation targets specific nerves rather than the spinal cord, showing superior results for localized extremity pain (81% success vs. 65% for SCS). Traditional opioid therapy remains an option but carries high risks of dependency and side effects. Compared to opioids, SCS offers a safer profile with significant reductions in drug usage, making it a preferred choice for many clinicians addressing the opioid crisis.
Does spinal cord stimulation hurt during implantation?
The trial phase involves sedation, so you should not feel pain during lead placement. Afterward, you may experience some soreness at the insertion sites. The permanent implantation is performed under general anesthesia or deep sedation, meaning you will not feel pain during the surgery. Post-operative discomfort is managed with prescribed medications and typically resolves within a few weeks.
Can I drive with a spinal cord stimulator?
Yes, most patients can drive once they are cleared by their surgeon, usually after the incision heals and pain medication no longer impairs reflexes. However, you must ensure the device does not interfere with your ability to react quickly. Some manufacturers recommend keeping magnets away from the IPG, so avoid strong magnetic fields near the device site.
Will my insurance cover spinal cord stimulation?
Most major insurers, including Medicare, cover SCS for approved conditions like failed back surgery syndrome and CRPS. Coverage usually requires documentation of failed conservative treatments and a successful trial period. Out-of-pocket costs vary widely, so check with your provider regarding deductibles and co-pays, which can range from $5,000 to $25,000.
How long does the battery last?
Battery life depends on usage and device model. Traditional IPGs last 5 to 9 years. Newer rechargeable systems may last 10 to 15 years with proper charging habits. Replacing the battery is a minor surgical procedure that does not require removing the leads.
What are the signs that the leads have migrated?
Lead migration often causes a shift in where you feel the tingling sensation or a complete loss of pain coverage. You might notice the stimulation moving to a new area or becoming inconsistent. If this happens, contact your pain specialist immediately. Minor adjustments can often fix the issue without additional surgery.